Warning: This story contains graphic descriptions of the practices involved in female genital mutilation
Shamsa Sharawe has become infamous within the Somali community across the world for speaking out against female genital mutilation (FGM) . In a video to illustrate what happened to her vulva when she was aged six she cut off the petals of a rose with a razor blade and then stitched up what was left of the flower.
The TikTok post went viral – with nearly 12 million views since it was shared 16 months ago.
No Somali, even in the diaspora, talks openly about FGM – never mind the problems that can come with it like painful periods, the difficulty of urinating, the agony of having sex and the dangers and trauma of giving birth when one’s vulva (including the lips and clitoris) have been cut off and the vaginal opening has been narrowed to a tiny hole.
This form of FGM – known as infibulation or “type three” – is what happens to most girls in Somalia as it is a commonly held belief that the cutting off their outer genitalia will guarantee their virginity.
Women who do not undergo FGM are regarded by many in Somali society as having loose morals or a high sex drive, which risks ruining a family’s reputation.
Yet the 31-year-old TikToker, who came to live in the UK in 2001 when her family fled Somalia’s civil war, is not afraid to take on such taboos with humorous, engaging and sometimes heart-breaking honesty.
Using the name Shamsa Araweelo on TikTok, she has shared a horrific account of how she was forcibly married off and raped not long after she turned 18 while on a trip to Somalia. It took six months for her to find a way to escape back to the UK.
But perhaps the biggest taboo of all has been to admit that she wanted her genitalia back – so much so that she has paid to have reconstructive surgery as it is not available to women through the UK’s National Health Service (NHS).
She found out that this was possible when she was contacted by Haja Bilkisu, a German citizen who had undergone FGM as a child on a visit to her birth country of Sierra Leone.
Responding to Ms Sharawe’s rose video, Ms Bilkisu explained that she had had her clitoris reconstructed thanks to Dr Dan mon O’Dey at Germany’s Luisenhospital in Aachen.
“I was terrified of the idea of re-cutting, even though this time it was with my consent,” Ms Sharawe tells the BBC.
“But I had to do it for my mental health. I just wanted to never feel pain again.”
The surgery includes the reconstruction of the clitoris and labia – in Ms Sharawe’s case using tissue from her buttocks – and the removal of cysts and scar tissue in order to reduce pain and restore a woman’s sex life. In some instances, the vaginal opening is also enlarged back to normal.
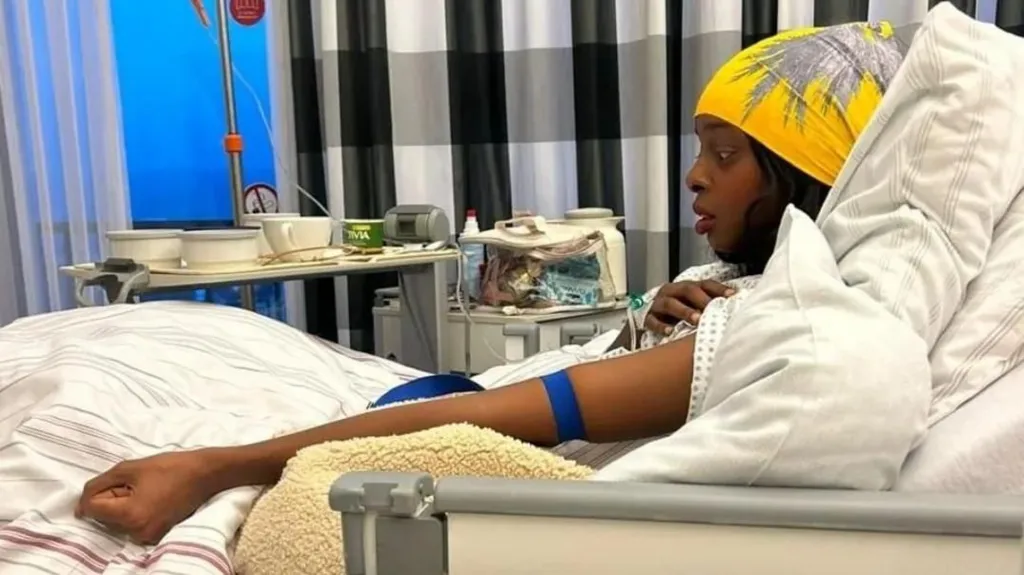
Ms Sharawe, who was featured in last year’s BBC list of 100 women for her determination to end FGM, decided to share her journey to Germany and recovery so other women like her could know their options.
Yet it has taken years of abuse and the trauma of a second failed marriage for her to find the courage to take on the establishment within the Somali community.
Ms Sharawe, now a single mother with a 10-year-old daughter, also feels let down by the NHS.
It only offers deinfibulation for FGM survivors – that is surgery that opens up the vagina, but does not replace any removed tissue and will not undo any of the damage.
Ms Sharawe decided to look for funds to pay for surgery in Germany.
Through online crowdfunding, she managed to raise £25,000 ($32,000) – and underwent a four-and-half hour procedure in December.
She was in Germany for three weeks and on her return, the anti-FGM activist and teaching assistant was not able to leave her house for months as she recovered.
The childcare costs and other expenses on top of the surgery mean she is still in debt – owing around £3,000 to the hospital.
“Paying for damage you didn’t choose for yourself, or you didn’t create, is really unfair,” she says.
There are four different types of FGM with varying levels of severity:
- Clitoridectomy: partial or total removal of the sensitive clitoris
- Excision: partial or total removal of the clitoris plus the inner skin folds surrounding the vagina (labia minora)
- Infibulation: cutting and repositioning of the outer skin folds around the vagina (labia minora and labia majora). Often includes stitching to leave only a small gap
- Covers all other harmful procedures like pricking, piercing, incising, scraping and cauterising the clitoris or genital area.
In the past couple of decades, medical techniques have been developed to try to repair the damage – pioneered in 2004 by French surgeon Dr Pierre Foldès.
Clitoral reconstruction is covered by public health insurance in Belgium, Finland, France, Germany, Sweden and Switzerland.
However, in Africa – where the majority of girls and women who have undergone FGM live – access to surgery is limited to Kenya, where patients must pay around £1,000, and Egypt, where non-governmental organisations can cover the costs.
“Not every surgeon can do this surgery. It’s complicated and every patient is different,” says Dr Adan Abdullahi, a specialist in Kenya.
But he says women with every type of FGM could benefit: “It has a positive effect on childbirth, especially for ‘type three’, which is associated with a narrowing of the vagina.”
Other issues, such as pain during sex, can be significantly improved or cured, he says – adding that his patients often experience improved self-esteem “and a sense of completeness”.
Ms Bilkisu says she does feel more complete since her surgery, which was covered by the German health system: “Undergoing surgery was really a power move, a way to fight back.”
But the 30-year-old recruitment agent encourages others to do their research thoroughly before deciding: “Reconstruction is not only to reconstruct the clitoris.
“A lot of women who are cut have thick scar tissue. You have to discuss it with your doctor. What can you do to make the vulva more elastic?”
Ms Bilkisu, who was determined to have “a normal sexual experience” one day and autonomy over her body, has had three operations over the last three years – each one taking around six hours.
“That’s tough on your body. You’re put under anaesthesia. You have to take medication afterwards. I couldn’t walk for three weeks,” she says.
The physical toll of such operations means some doctors, like Dr Reham Awwad in Egypt, are keen to promote non-surgical procedures.
The co-founder of the Restore clinic says that although reconstruction surgery can bring relief, the cutting is sometimes so severe that even the most advanced surgical techniques cannot restore sexual function.
“I definitely don’t think surgery is the answer for everyone,” she tells the BBC.
Around half the cases at her clinic, which opened in 2020, are now treated using non-surgical means like injections of platelet-rich plasma which promotes tissue rejuvenation.
“The plasma [can] lead to regeneration and stimulation of increased blood flow and reducing inflammation in the areas where you inject it,” she says.
However, she cautions that the high cost means such treatments are beyond the reach of many.
Her clinic also offers psychological therapies to overcome trauma for women cut at an age when they can remember the experience.
For those who do opt for reconstructive surgery, the results can be emotional.
“The first time I actually saw my clitoris I was taken aback because for me it was like this doesn’t belong to me,” said Ms Bilkisu, who was eight years old when she underwent “type two” FGM.
Ms Sharawe agrees it takes some getting used to, plus learning how to deal with things like proper period bleeds.
It will take her another six months to completely recover – and she has not been able to afford to go back to Germany for a check-up, which worries her.
“But now I know how it feels to be a full woman… I am a very happy woman,” she says.
“I can wear underwear without discomfort or pain. I can wear trousers. I feel normal.”
And while she has experienced an expected backlash from some Somalis on social media – some of her family have surprised her with their support.
One of her uncles even wanted to know if the surgery was available in the UK for his wife.
“He didn’t feel comfortable knowing his wife’s FGM was still affecting her even after 50-plus years. He wanted to improve the quality of her life… because we [all] deserve to have a good quality of life.”














